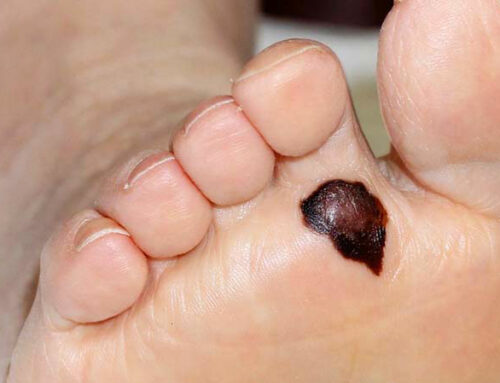
An observational study to determine best practice based on clinicians’ reported management of NSW melanoma patients over a 12-month period.
This is a population-based, observational study based on clinicians’ reported management over a 12-month period of melanoma patients across New South Wales. The aim was to assess the patterns of medical care for patients against best practice guidelines and identify any variations and therefore areas for improvement. Once the Cancer Registry received notification of a new diagnosis of melanoma, the referring doctor was sent a questionnaire and similarly with any other
clinicians subsequently involved in the patient’s care. Over 70% of clinicians responded and almost 4,000 questionnaires were received, providing data for about 2,700 patients.
This has been an ambitious and very productive study done in collaboration with The NSW Melanoma Network with three papers accepted, another two under revision with the journal and three more in preparation. Just a handful of the more interesting findings include:
- Adherence to clinical guidelines for surgical management and follow-up is not what it should be. Surgical margin guidelines were only adhered to in 35% of cases, while 45% were over-treated and 21% under-treated. Such factors as clinician caseload, age and socio-economic status of practice location were associated with variations.
- 74% of patients’ doctors were aware of their risk factor status with respect to personal and family history of melanoma and the presence of moles. Doctors were more likely to know the family history of younger melanoma patients (under 40) than those over 80 and were more likely to give early detection advice to the younger age group.
Clinical management of higher risk patients was more likely to conform to best practice guidelines for diagnosis and skin surveillance than that of lower risk patients.